Inês Azevedo1, Helena Torrão2, Ana Maia Ferreira3, Iris Maia3, Miguel Costa1
1Pediatric Department of Centro Hospitalar de Entre Douro e Vouga, Portugal, 2Radiology Department of Instituto Português Oncologia do Porto Francisco Gentil, Portugal, 3Pediatric Department of Instituto Português Oncologia do Porto Francisco Gentil, Portugal
Address for Correspondence: Inês Alexandra Azevedo, Avenida da Misericordia n79 4º direito, 3700-192 São João da Madeira, Portugal.
Email: Inesaazevedo1995@gmail.com
|
Question :An eight-year-old female, previously healthy, was examined by a pediatrician due to a left axillary swelling that persisted for four weeks. This mass was noticed two weeks after receiving the first dose of the anti-SARS-CoV-2 vaccine. The patient denied experiencing other symptoms, trauma or recent infections. During the physical examination, a firm oval mass measuring 5x5 cm was observed, with no signs of inflammation (Figure 1).
She underwent an analytical study without any peculiarities and an axillary ultrasound, revealing an oval mass with multiple indentations and hypoechoic elements. This pattern suggested an atypical adenopathy conglomerate in the context of a vaccine reaction. Consequently, she initiated treatment with a seven-day course of amoxicillin + clavulanic acid and ibuprofen.
On re-evaluation, there was no change observed in the mass. Consequently, the case was reviewed with Pediatric Oncology and a referral for consultation was made. A repeat axillary ultrasound revealed a heterogeneous formation with cystic foci and areas of vascularization, accompanied by rare foci of calcification (Figure 2). Subsequent Magnetic Resonance Imaging (MRI) confirmed the presence of a lesion consistent with low-flow vascular malformation within the teres minor muscle (Figure 3). The child underwent surgical excision and histology confirmed the diagnosis of intramuscular hemangioma (IMH).
Figure 1. Oval mass in left axile, with 5 x 5 cm.
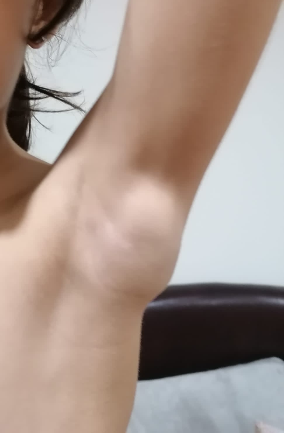 Figure 2.
Figure 2. Ultrasound images showing heterogeneous formation, with cystic foci (A) and areas of intralesional vascularization (B), with rare foci of calcification.
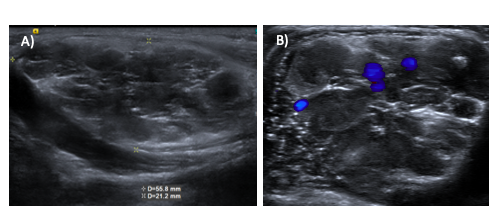 Figure 3.
Figure 3. A) MRI Axial T1 imaging showing lesion, with lobulated contours, within left teres minor muscle, demonstrating intermediate signal; B) MRI Axial STIR viewing lesion with hypersignal, plus foci of hyposignal; C) MRI Axial imaging after contrast, showing heterogeneous impregnation of contrast product in the lesion.  What is intramuscular hemangioma?
|
Discussion :
Hemangioma is a frequent benign tumor, representing about 10% of soft tissue tumors. 1 However, IMH is uncommon, accounting for less than 1% of all hemangiomas. 1 IMH is a vascular benign proliferation that occurs within the muscle and the most frequently affected sites are the lower extremities. 2 The prevalence of IMH in the rotator cuff muscle is unknown and only a few reports are described in the literature. 3,4,5
Hemangiomas are common benign tumors, comprising approximately 10% of all soft tissue tumors. 1 However, Intramuscular Hemangioma (IMH) is rare, constituting less than 1% of all hemangiomas. 1 IMH is characterized by a vascular benign proliferation within the muscle, with the lower extremities being the most frequently affected sites. 2 The prevalence of IMH in the rotator cuff muscle remains unknown and only a limited number of reports are available in the literature. 3,4,5
In physical examination, it manifests as an infiltrative mass characterized by slow growth, displaying variable size and coloration. 1 These signs are non-specific and may be observed in other pathologies, leading to a potential diagnostic dilemma. 2 While MRI is essential for diagnosis, confirmation is achieved through the histology of the excised tumor. 3 In the case of Intramuscular Hemangioma (IMH), the standard treatment is surgical excision with the aim of achieving clear margins. 1
In summary, in this clinical case, the onset of symptoms following vaccine administration can complicate the assessment and diagnosis of other pathologies. Therefore, when confronted with persistent swelling and alarming signs, it is crucial to systematically rule out other potential causes. | References : | - Lescura CM, de Andrade BAB, Bezerra KT, Agostini M, Ankha MVA, de Castro F, Carvalho YR, Romañach MJ, Anbinder AL. Oral intramuscular hemangioma: Report of three cases. J Cutan Pathol. 2019 Aug;46(8):603-608. doi: 10.1111/cup.13482. Epub 2019 May 9. PMID: 31006896.
- Lee HS, Hong YC, Jung KJ, Yeo ED, Won SH, Jang SH, Ji JY, Lee DW, Yoon SJ, Kim WJ. A Huge Plantar Intramuscular Hemangioma in the Plantar Area Treated Surgically: A Case Report and Literature Review. Int J Environ Res Public Health. 2021 Aug 28;18(17):9088. doi: 10.3390/ijerph18179088. PMID: 34501676.
- Ki Won Lee, Hyun Il Lee, Chung Hwan Kim, Tae Kyung Kim. Large Cavernous Hemangioma of the Subscapularis Muscle: A Case Report. Clinics in Shoulder and Elbow. 2014;17(4):185-189. DOI: https://doi.org/10.5397/CiSE.2014.17.4.185.
- Lin, Heng-Tai & Hong, Chih-Kai & Jou, I-Ming & Tsai, Hung-Wen & Su, Wei-Ren. (2016). Intramuscular Hemangioma of the Subscapularis Muscle Presenting with Isolated Loss of External Rotation of the Shoulder. International Journal of Orthopaedics. 2. 512-514. 10.17554/j.issn.2311-5106.2016.03.146.
- Abu-Ghname A, Luu BC, Trost J, Raj S, Truong L, Davis MJ, Desai SB, Pederson WC, Maricevich M, Maricevich RS. The Challenges of Upper Extremity Intramuscular Hemangioma: A Case Study and Systematic Review. Plast Reconstr Surg. 2022 Aug 1;150(2):367-376. doi: 10.1097/PRS.0000000000009324. Epub 2022 Jun 8. PMID: 35671450.
|
|
| Correct Answers : |  100% 100% |
Last Shown : Mar 2025
|